Otolaryngology (“ENT”), allergy, and asthma (“ENTA&A”) related medical practices have been enjoying a robust period of investor interest as private-equity backed physician-practice management (“PPM”) companies and health systems have sought to align with providers in this sector. With opportunities for multiple ancillary offerings such as audiology and hearing aid sales, to the ability for ENT physicians to perform outpatient surgeries in an ambulatory surgery center (“ASC”) setting, there will likely be continued investor interest in this sector for years to come. This article discusses the key drivers to transaction activity in the ENTA&A sector, provides insight into the current transaction environment, and outlines the value proposition that different buyers typically bring to a potential transaction.
![]() ENT SPECIALTY OVERVIEW
ENT SPECIALTY OVERVIEW
ENT physicians can function as generalists or choose to complete additional training in areas of Ear, Nose, Throat, Head and Neck, Thyroid, Sleep, Pediatrics, and Facial Plastic and Reconstructive Surgery.[1] Example conditions treated by ENT physicians include:[2]
![]() Ear Conditions, including ear infections, tinnitus, dizziness, vertigo, hearing loss, ruptured eardrum, otosclerosis, and eustachian tube dysfunction;
Ear Conditions, including ear infections, tinnitus, dizziness, vertigo, hearing loss, ruptured eardrum, otosclerosis, and eustachian tube dysfunction;![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()

![]() ALLERGY AND ASTHMA SPECIALTY OVERVIEW
ALLERGY AND ASTHMA SPECIALTY OVERVIEW
Allergy and Asthma physicians are involved in the diagnosis and treatment of certain medical issues and conditions, some of the more common of which are outlined below:[3]
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]()
![]() TRANSACTION ENVIRONMENT
TRANSACTION ENVIRONMENT
Figure 2 illustrates annual transaction volume for ENTA&A practices in the United States from 2017 through 2023. We note that the data presented has been sourced from a single transaction database and is not meant to represent total ENTA&A transaction volume, but to serve as a proxy for recent increased transaction activity. We note that most ENTA&A transactions are private and not publicly disclosed.
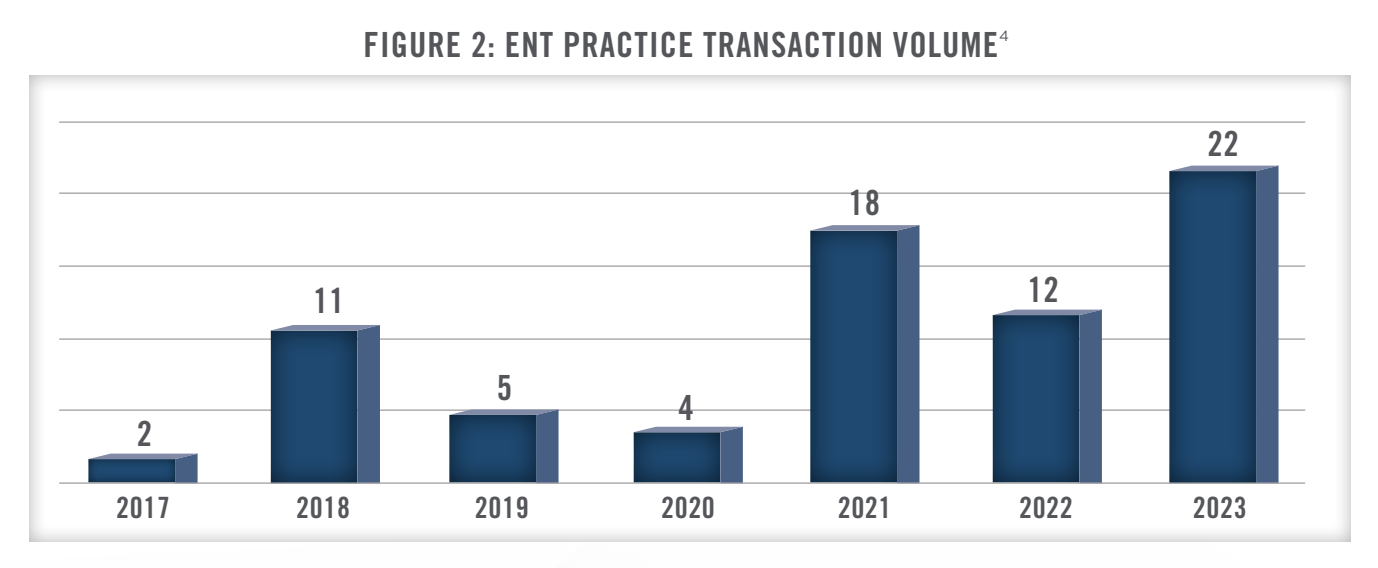

Transaction activity has increased over the last several years as PPM investors in the sector have increased, and sellers see the valuation proposition of partnering with a management organization or health system. For an independent medical group, the administrative burden, staffing pressures, inflation, and difficult reimbursement environment can all play a factor in a group deciding to partner with a PPM or health system. As outlined in Figure 3, while changes in Medicare reimbursement in the ENTA&A sector were positive in 2021, other recent years were generally flat or negative.
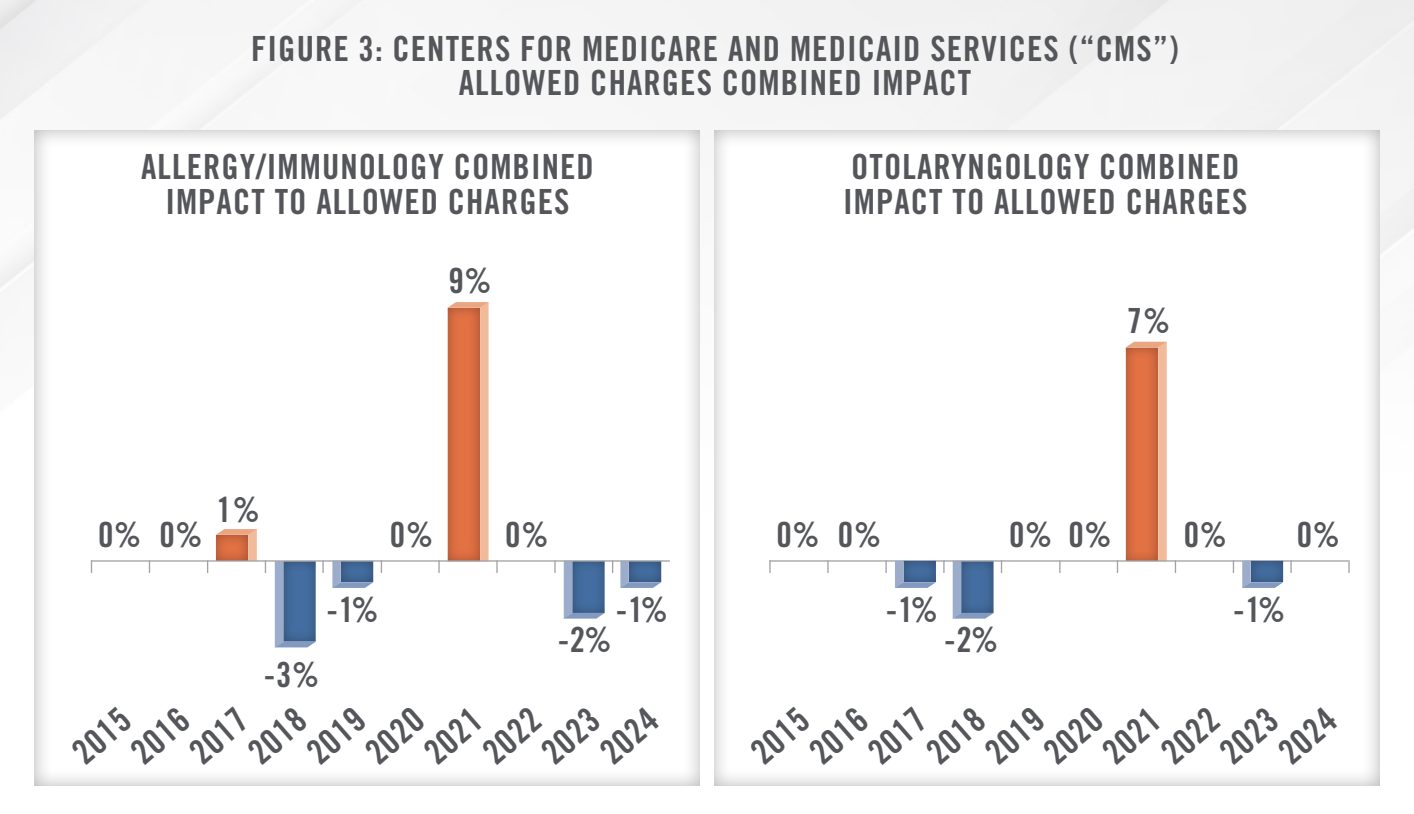

Compensation for ENTA&A physicians has increased at nominal levels in recent years, with an approximate compound annual growth rate of approximately 1.8 percent for the four-year period ended 2022, based on our review of median compensation reported by MGMA[5] for the specialties of Allergy/Immunology and Otorhinolaryngology. Reimbursement from governmental payors that has not kept up with inflation, paired with inflationary pressures on staff wages and supplies expenses that we have observed, are likely the culprits of fairly stagnant compensation levels for ENTA&A physicians in private practice.
Some of the financial and administrative challenges faced by independent practices can result in an opportunity for a health system or PPM partner. While acquisitions in the ENTA&A sector in recent years have started a trend toward industry consolidation, there still appears to be fragmentation in the sector. While the number of otolaryngologists increased approximately 18 percent between 2014 and 2021, the number of practices fell approximately 12 percent during the same period. While a PPM or health system partner can typically assist in addressing burdens associated with items such as negotiating favorable payor contracting, they may also have the experience and expertise to start or expand new ancillary service lines. Ancillary income streams in an ENT practice often includes sources such as those outlined in Figure 4.
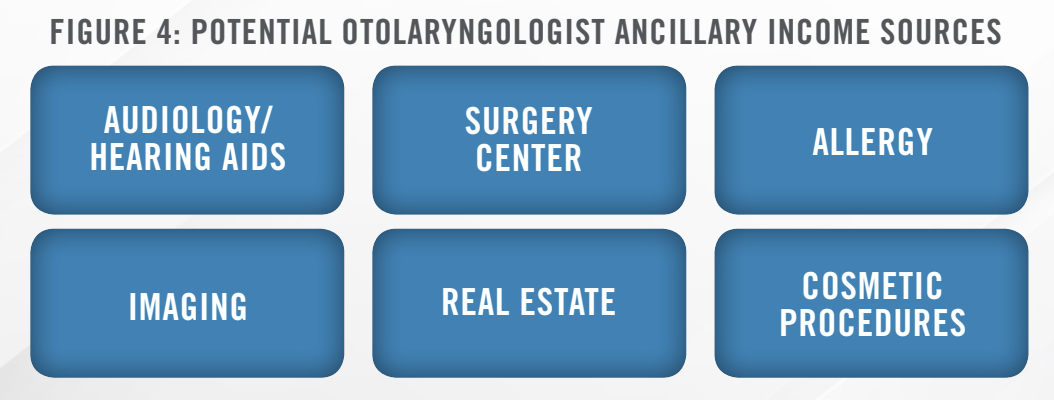

Surgery Centers
Surgery Centers can be a notable source of ancillary income for otolaryngologists. Figure 5 depicts EBITDA margins for ASCs based on HealthCare Appraisers’ 2021 ASC Valuation and Benchmarking Survey.
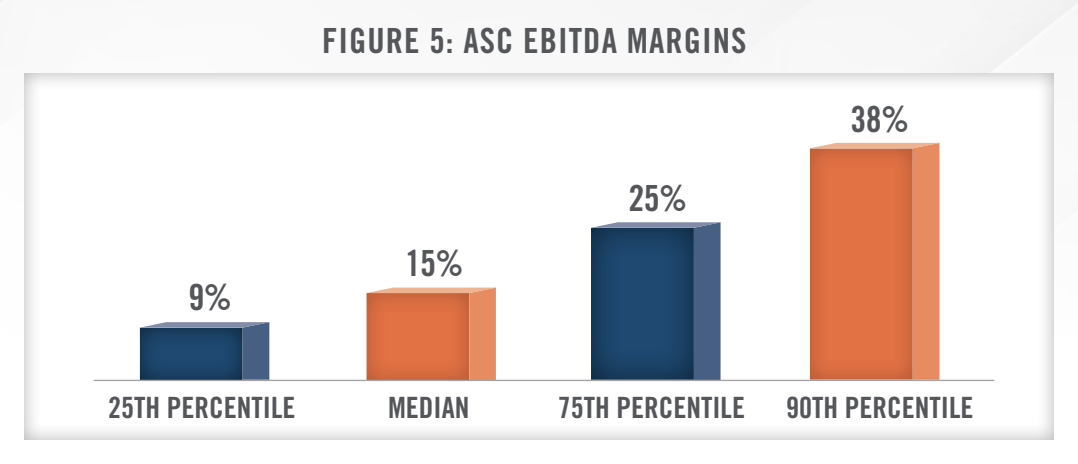

A broad-based trend in healthcare has been a shift in cases from a hospital-based setting to an ASC setting. In the otolaryngology sector, we note that ASCs have been going in-network with payors to perform Inspire sleep apnea cases, which are generally anticipated to be financially lucrative to an ASC on a contribution margin basis. However, given the expensive device cost in performing these procedures, regional differences in Medicare reimbursement may result in profitability challenges in performing these cases in the ASC setting. This topic was discussed at a presentation given by Inspire Medical Systems (NYSE: INSP) at The Stifel 2023 Annual Healthcare Conference:
And the challenge is while Medicare will reimburse fairly in the major cities and primarily in the North here in New York, the ASCs pay very, very well. You get into the south in the Mississippi and Alabama, it can put the ASC into a loss position with Inspire, and that’s going to create a challenge. It all is based on the way that CMS does device-dependent procedures where they discount not only the labor rates, but they discount the material as well, and that’s unfair…. Most ASCs can handle commercial cases, if they have a contract, they have to do individual contracts United, Anthem, Aetna. And once they get them in place, it is a profitable position for the ASC, but it’s difficult for a surgeon to say, I’m going to do all the Medicare at the hospital and now I’m going to take all the private over to my ASC, where it’s profitable.
Hearing Aids
Hearing aids have traditionally been a notable ancillary income source for otolaryngology practices.[6] However, the U.S. Food and Drug Administration issued a final rule in 2022[7], effective October 17 of that year, which established the ability for consumers to purchase over-the counter (OTC) hearing aids for adults with mild to moderate hearing loss. While some sources suggest the financial impact of this change is still playing out,[8] it highlights an overarching broad trend of federal regulation that continues to impact the delivery of healthcare in the United States, and that practices need to be continually adaptive to this changing environment to avoid potentially negative financial ramifications.
Allergy and Asthma
Another trend we have broadly observed in healthcare post-COVID involves a shift towards patient care that is convenient and cost effective – in their homes. In the allergy and asthma sector, we have observed a shift in the administration of biologics to treat severe asthma from the office to the home setting.[9]
Additionally, we note increasing instances of asthma in the United States. The Centers for Disease Control reported that the percent of the U.S. population with asthma has increased from 7.4 percent, or approximately 20.3 million people in 2001, to 7.7 percent of the population, or approximately 25.0 million people, in 2021.[10] Impacts of seasonal allergies are also on the rise. A study spanning 1990 to 2018 found that pollen seasons are starting 20 days earlier, and lasting 10 days longer, and feature a 21 percent increase in the amount of pollen.[11] Overall, nearly one in three U.S. adults and more than one in four U.S. children reported having a seasonal allergy, eczema, or food allergy in 2021.[12]
![]() VALUATION MULTIPLES
VALUATION MULTIPLES
PPM acquisition multiples of medical practices can vary greatly, with factors such as size of the group, location, ancillary offerings in place, and growth outlook being a few of the factors that can impact transaction consideration. Based on our experience observing closed PPM transactions, in many instances, small to mid-size groups are likely to attract EBITDA multiples in the mid-to-high single digits, with large, platform acquisitions commanding double digit multiples, as displayed via the examples in Figure 6.


Health system transactions tend to differ from PPMs in that health systems typically focus their offers on employment contract compensation, as compared to the levels of upfront transaction consideration offered by PPMs. Some notable transactions in the ENTA&A space over the last year are presented in Figure 7.
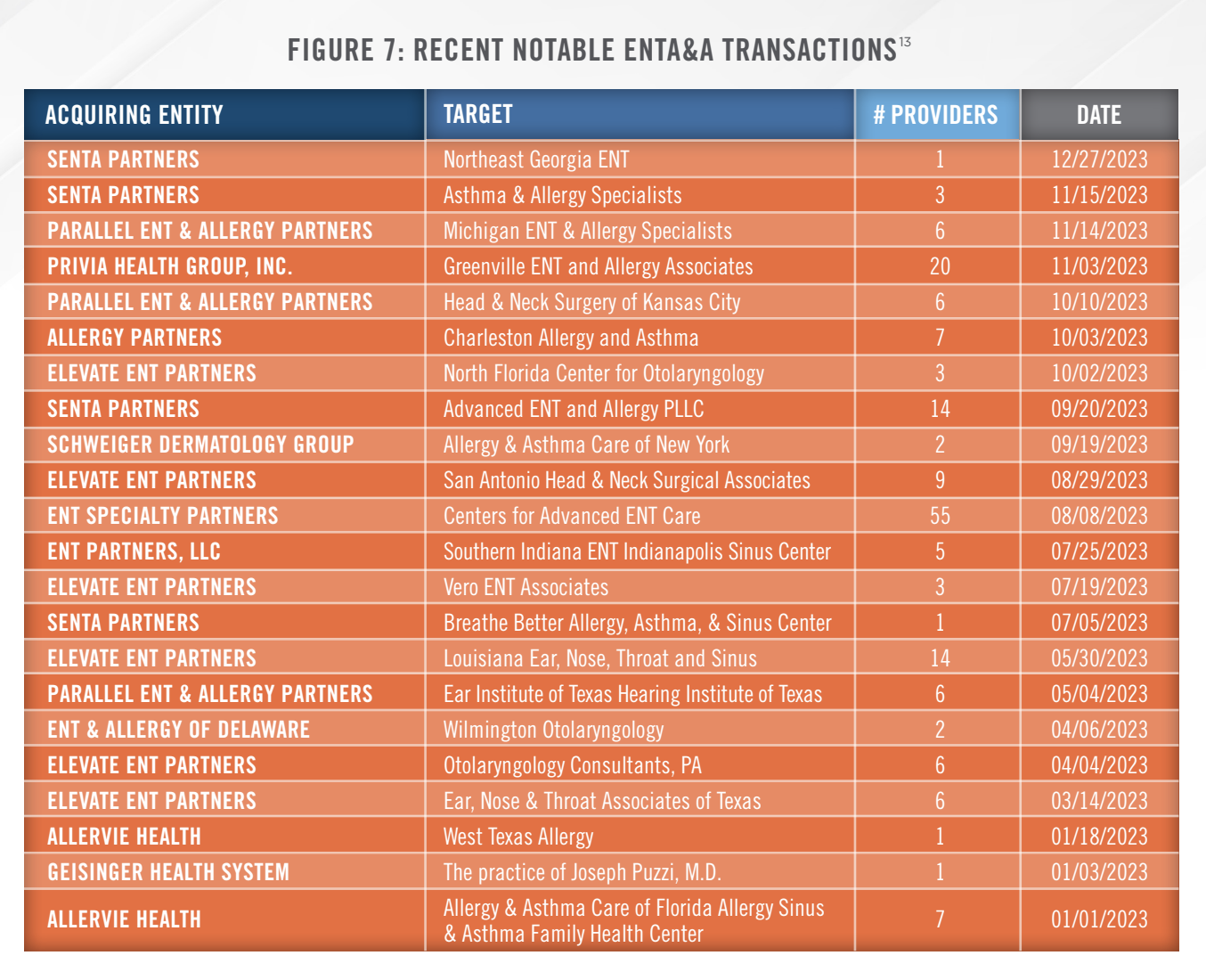

Major active PPM companies presently have operations in several areas of the United States as shown in Figure 8.
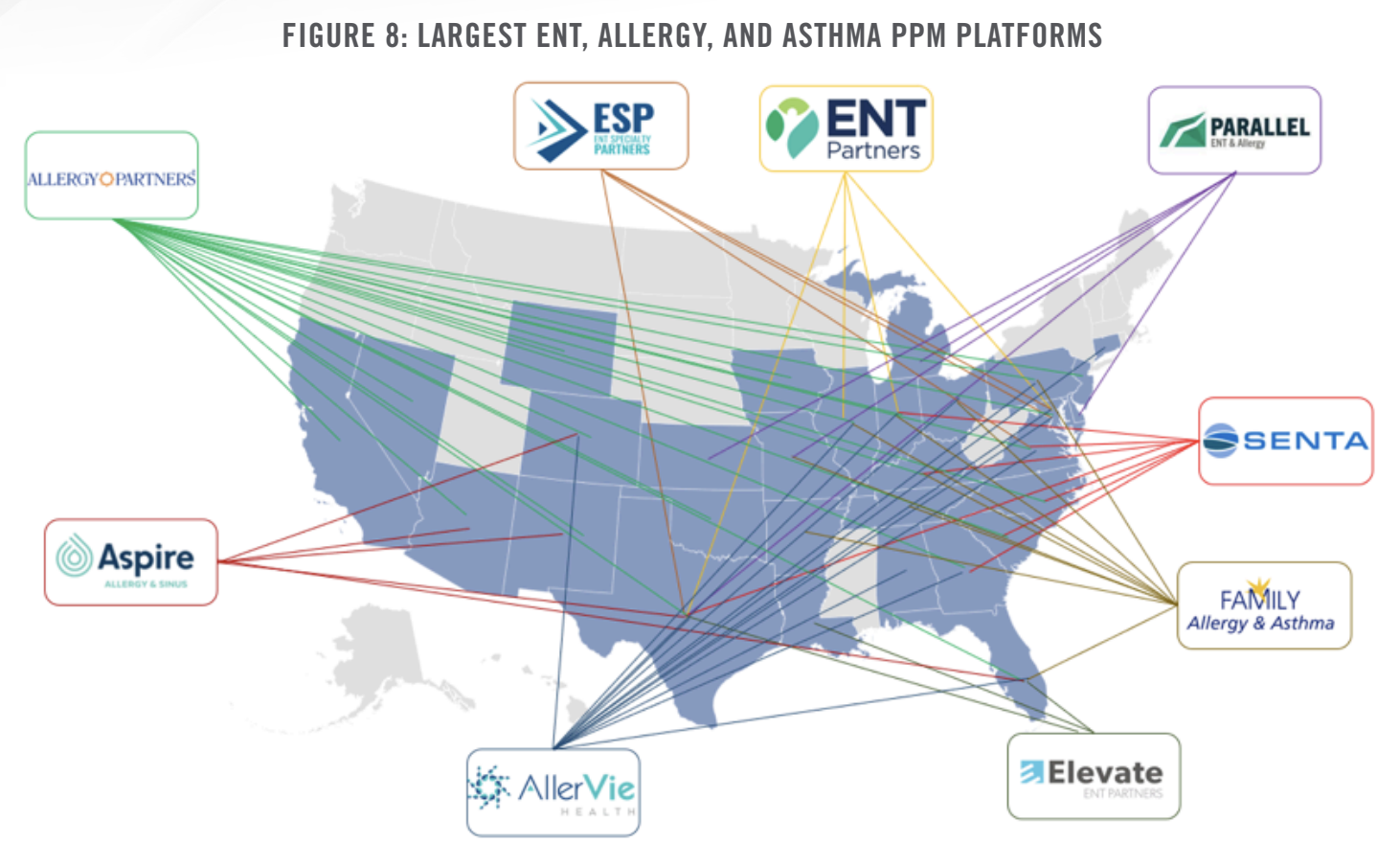

How Different Buyers Approach Transactions
Based on our involvement with physician practice transactions involving private equity-backed PPMs, a common strategy involves the owner physicians of the target practice agreeing to take a “scrape” (i.e., pay cut) post transaction, which increases EBITDA on an adjusted basis, and, in turn, purchase price. Figure 9 depicts an example of a scrape and the coinciding purchase price in a hypothetical transaction.


Under this transaction approach, physicians sacrifice annual compensation in exchange for a higher upfront purchase price. We note that a portion of the upfront purchase price is typically paid as rollover equity in the post-transaction business, which typically ranges from 20 to 40 percent of the total purchase consideration. The provision of rollover equity incentivizes the physician group to stay engaged post transaction as a second lucrative payment can be achieved should the PPM sell the medical group for a high exit multiple. These higher exit multiples can be achieved through organic growth and the PPM’s willingness to invest in the addition of ancillary services (ASCs, OBLs, etc.) post transaction. Many smaller physician groups lack the capital needed to build and develop these ancillary services on their own, which motivates them to enter into an agreement with a PPM. Physician involvement in a transaction with a PPM does carry risk, as the rollover equity could potentially decrease in value depending on how the PPM is able to execute both on its ability to roll-up additional ENTA&A medical groups into its PPM, as well as its ability to grow the revenue and/or profitability of the groups that comprise the PPM. Rollover equity is another item that makes it difficult to compare a PPM transaction to a health system transaction.
We note that physicians do not solely inherit risk by partnering with PPMs. A PPM typically manages all of the non-clinical administrative work post transaction, which allows the physicians to focus on providing the best care possible for their patients without the burden of managing the business aspects of a medical practice. The ability to leverage the C-suite of a PPM can allow a practice to grow in ways that many would not be able to achieve on their own.
Conversely, health systems tend to approach physician groups with lower upfront purchase prices but higher ongoing compensation packages. Based on the health systems we have worked with, posttransaction compensation tends to be tied to productivity (typically a compensation per wRVU metric), which rewards physicians for high productivity and motivates them to continue building their practices. The dynamics vary depending on the physician group’s compensation pre transaction, with some health system transactions still commanding upfront purchase prices above tangible asset value as the target physician groups historically were compensated at high levels. Another important item to note is that the compensation health systems pay the physicians post transaction must be consistent with fair market value (“FMV”). Should the target physician group already have high compensation levels, the health system may be constrained by FMV and not be able to provide a higher compensation package. In many instances, this is the result of practices in which there are many employed physicians, Advanced Practice Providers, and in-office ancillary services, allowing owner physicians to earn high levels of compensation compared to peers producing at similar levels of personally performed services. Figure 10 highlights a scenario where a physician group receives a higher compensation package, while Figure 11 highlights a scenario where FMV constrains the ability of the health system to increase compensation post transaction.


As highlighted in the figures, purchase price and post-transaction compensation are inversely related. Transactions involving health systems typically leave the physician group with different risk than transactions involving PPMs. While there is uncertainty surrounding the future value of rollover equity and achieving of income repair in a PPM transaction, uncertainty surrounding the future compensation levels under an employment contract, which are typically governed by what compensation level is FMV, can be a risk factor under a health system transaction.
Potential Impacts of FTC Proposal to Ban Non-Compete Agreements
On January 5, 2023, the Federal Trade Commission (“FTC”) proposed a rule that would ban noncompete agreements if enacted. If put into effect, employers would be barred from entering into future noncompetes with employees and all noncompete agreements currently in effect would be disbanded. The major exception to this proposed rule is that transactional noncompete agreements would still be allowed for those who own a 25 percent or greater interest in the subject business of the transaction.[14] We also note that this is only a proposed rule by the FTC that will need to go through a commentary and review process. Following the commentary and review process, a majority vote of the FTC commissioners will be needed to finalize the rule. Even after going final, there is the potential for legal challenge that could delay or block the enactment of the rule. The vote has already been delayed, pushed to an April 2024 date. Ultimately, the impact on how this potential new rule may impact acquisition activity of ENTA&A medical practices is uncertain. However, one could speculate that the absence of enforceable noncompete agreements for physicians in medical practice transactions may result in transactions involving more payback provisions, earnouts tied to achieving certain operational and/or employment milestones, and/or other deferred retention and incentive plans tied to certain post-transaction metrics.
![]() CONCLUSION
CONCLUSION
The ENTA&A space should continue to enjoy a strong demand for services, and consolidation in the industry should likewise continue. While we note the rising interest rates in 2023 have been a headwind for transaction activity in general, the future appears positive for acquisition activity to rebound, as the Federal Reserve is expected to cut rates several times in 2024.[15] A transaction has the opportunity to be mutually beneficial for both the physician sellers, as well as a PPM or health system acquirer. As sellers, physicians can shift their focus from the administrative burdens of managing a practice, to clinical care of their patients. Meanwhile, PPMs and health systems can use their size and administrative expertise to help alleviate the burdens of practice management and capital investment decision making.
CONTACT THE EXPERTS AT HEALTHCARE APPRAISERS TO DISCUSS YOUR ADVISORY AND VALUATION NEEDS REGARDING ANY CONTEMPLATED ACTIVITY IN THE ENTA&A SPACE.
NICHOLAS J. JANIGA, ASA
PARTNER
(303) 566-3173
NJANIGA@HCFMV.COM
MATTHEW MULLER, ASA
DIRECTOR
(303) 566-3179
MMULLER@HCFMV.COM
[1] Obtained from https://www.enthealth.org/whats-an-ent/ Last accessed February 3, 2024
[2] Obtained from: https://my.clevelandclinic.org/health/articles/24635-otolaryngologist Last accessed February 3, 2024
[3] Obtained from https://acaai.org/do-you-need-an-allergist/what-does-an-allergist-treat/ Last accessed February 3, 2024
[4] LevinPro HC, Levin Associates, 2024, January, levinassociates.com.
[5] Obtained from DataDive by Medical Group Management Association
[6] Obtained from: https://www.entnet.org/wp-content/uploads/2023/07/2022-Otolaryngology-Workforce.pdf Last accessed February 3, 2024
[7] Obtained from: https://www.federalregister.gov/documents/2022/08/17/2022-17230/medical-devices-ear-nose-and-throat-devices-establishingover-the-counter-hearing-aids Last accessed February 3, 2024
[8] Obtained from: https://www.medpagetoday.com/surgery/otolaryngology/104711 Last accessed February 3, 2024
[9] Obtained from: https://www.managedhealthcareexecutive.com/view/several-biologics-to-treat-severe-asthma-can-be-self-administered-at-homepatients-prefer-it Last accessed February 3, 2024
[10] Obtained from: https://www.cdc.gov/asthma/asthma-prevalence-us-2023-508.pdf Last accessed on February 3, 2024
[11] Obtained from: https://www.nifa.usda.gov/about-nifa/impacts/yes-allergy-seasons-are-getting-worse blame-climate-change Last accessed February 3, 2024
[12] Obtained from https://www.cdc.gov/nchs/pressroom/nchs_press_releases/2022/20220126.htm Last accessed February 3, 2024
[13] LevinPro HC, Levin Associates, 2024, January, levinassociates.com.
[14] University of Maryland Francis King Carey School of Law, “The FTC’s New Noncompete Proposal: A Potential Win for Workers and Possible Mass Changeover Across All Industries?” Last accessed February 3, 2024, https://www.law.umaryland.edu/content/articles/name-659569-en.html
[15] Obtained from: https://www.cnbc.com/2023/12/13/fed-interest-rate-decision-december-2023.html Last accessed February 3, 2024

